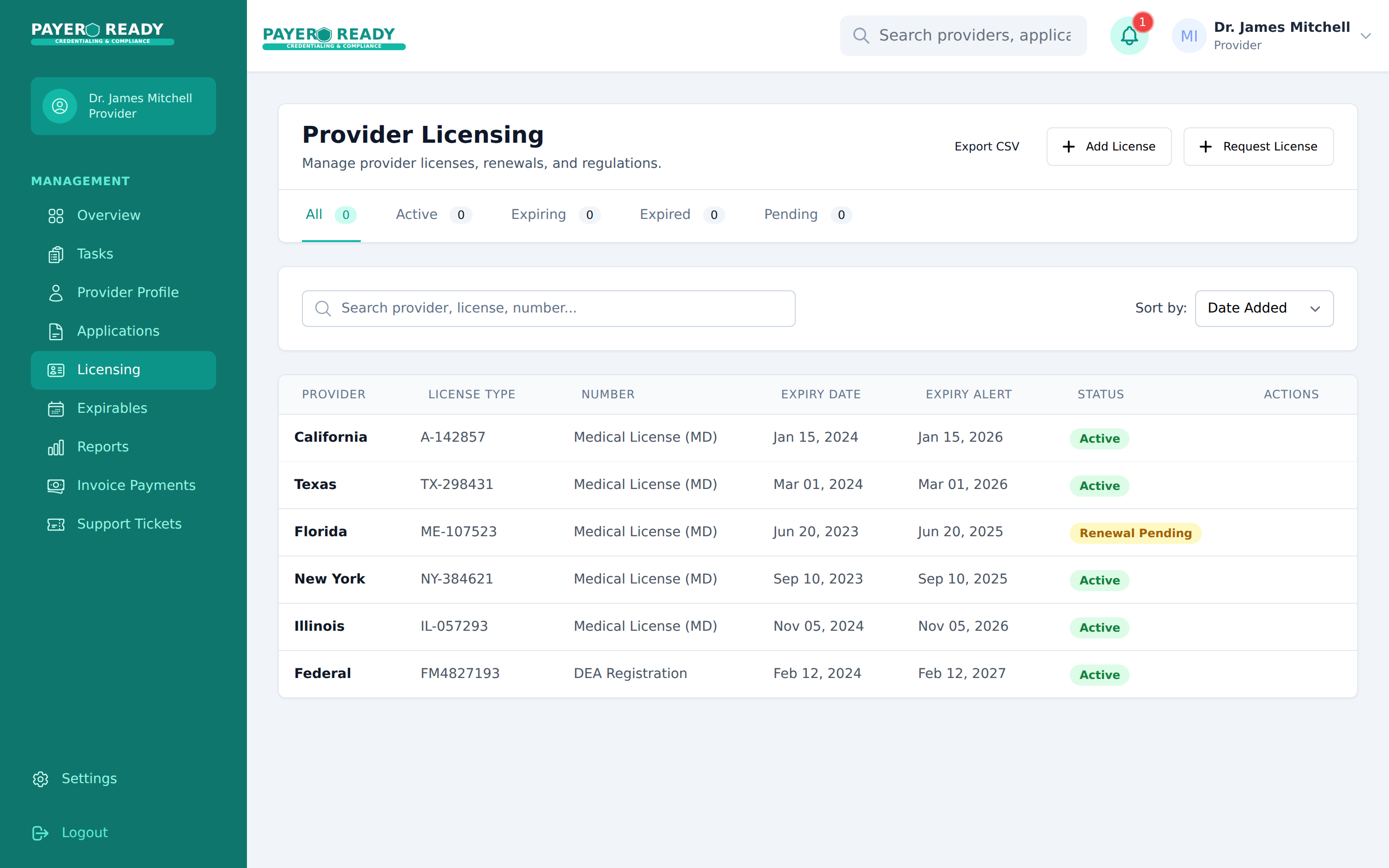
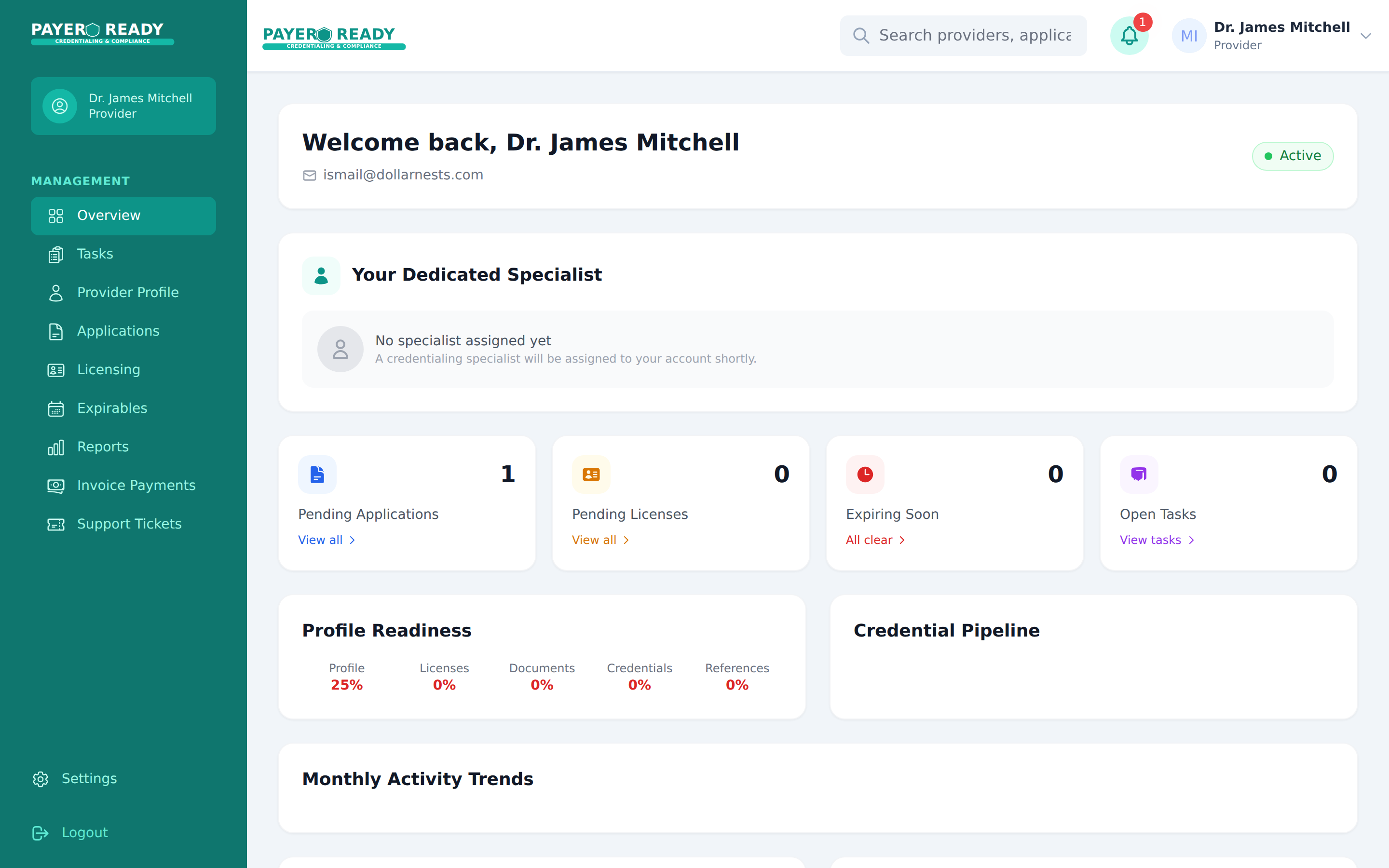
Credentialing Software Comparison: A 2026 Buyer's Guide for Practice Managers
Credentialing software is not one category. This guide splits the market into 5 distinct software types, explains what each actually does, covers pricing patterns, and helps practice managers decide whether they need software at all or a managed service instead.